Why We Should Not Be Concerned About Increasing Covid-19 Cases in Texas
Edward Peter Stringham
 Should we be concerned about the total number of COVID-19 deaths or COVID-19 cases that do not result in death? On June 29, 2020, former New York Times reporter Alex Berenson, and an important alternative voice on COVID-19, received a note from a managing partner of the medical care facilities CompleteCare in Texas. The author tells of what’s happening on the ground, and it differs dramatically from the headlines driving Texas officials to once again close up the economy in a panic over a rise in cases. Should we be concerned about the total number of COVID-19 deaths or COVID-19 cases that do not result in death? On June 29, 2020, former New York Times reporter Alex Berenson, and an important alternative voice on COVID-19, received a note from a managing partner of the medical care facilities CompleteCare in Texas. The author tells of what’s happening on the ground, and it differs dramatically from the headlines driving Texas officials to once again close up the economy in a panic over a rise in cases.
Recall that the original idea of “flattening the curve” was not to make the virus go away but to slow the spread of infections to prevent hospitals from getting overwhelmed in the short run (this was never an issue in Texas). The stay at home order for two weeks was meant to buy time for hospitals to get enough equipment and deal with patients over time rather than all at once. The good news is the hospitals were never overrun.
It also turns out that COVID-19 deaths were a fraction of the most alarmist predictions that drove public policy, and over time that COVID-19 deaths continue to decrease.
But now we hear about rising cases – not deaths – and that is introducing more calls for lockdowns and travel bans.
What the letter reports will not shock anyone who has followed cases during the reopening period. The cases are mostly young people who are in very little danger from the virus. What should be considered good news – that the case fatality rate is falling each day – is being misinterpreted by the press.
As for this gentleman’s willingness to speak out, it is a heroic act in these strange times. He worries of becoming a target and it is a legitimate concern. Even so, the truth needs to come out. AIER gives the letter, originally postedon Berenson’s twitter feed, a full airing.
Good morning,
I am the Managing Partner and General Counsel of a Texas based company that owns and operates 13 free-standing emergency clinics in the State of Texas. I follow your reporting and wanted to share with you some information on Texas. I want people to hear this story as opposed to the mainstream reporting. However, I am sensitive about putting a target on myself or my company for conveying this information. I am not sure how you’ve handled this type of situation but I suspect you’ve had other people send you information who are concerned about becoming a target.
In June, we tested over 2,231 patients (data through last Thursday). Positive rate is now close to 20% (was 4-6% in May). Vast majority of the cases are mild to very mild symptoms. Average age of the people getting tested in mid-30s.
Very different patient (in terms of age) than we’ve seen before June. Most of these patients would not have met criteria that we previously had (and all the health facilities had) for Covid testing. Now with more testing kits we are able to test a broader group of patients.
Clinically, we’ve had very few hospital transfers because of Covid. Vast majority of the patients are better within 2-3 days of the visit and most would be described as having a cold (a mild one at that) or the symptoms related to allergies. We’ve often provided a steroid shot and some antibiotics. By the time we have follow-up calls, most of the patients are no longer experiencing any symptoms. They often say the shot really made a difference.
In terms of what is driving them to the ER — Roughly 1/2 have been told by their employers to get a test. They have a sneeze or a cough and their employer tells them to go get tested. The other 1/2 just want to know. They have mild symptoms (and some don’t have any symptoms but game the system and check a box that they have a symptom so they can get a test — they cannot get a test unless they present with symptoms. If they have no symptoms we send them away — which does happen.)
The average length of stay of Covid patients is 3-5 days. Much lower than the patients being seen in April and early May. Their symptoms are also milder. Most of the patients are not ending up in the ICU. The hospital ICUs are filled with really sick people with non-Covid issues.They [didn’t] come in earlier because they were scared and now they are super sick. From multiple sources at different hospitals — they have plenty of capacity and no shortage of acute care beds.
No real data on breakdown of patients who have Covid but are not in the hospital because of Covid. Recognition that because all patients are tested for Covid you have some percentage of patients listed as Covid patients who are non Covid symptomatic and that the hospitalization rate is somewhat driven by hospitals taking their normal patients with other medical issues.
Finally, heard several stories of how discharge planners are being pressured to put Covid as primary diagnosis — as that pays significantly better. Hospitals want to avoid the discussion but if they don’t they risk another shutdown. This may be an explanation for why there is a gap in hospital executives saying they have plenty of capacity and the increasing number of Covid hospitalizations. You open up your hospitals for normal medical care and you test everyone (sic) of those patients — the result is higher percentage of patients who have Covid — now.
Overall, based on what we are seeing at our facilities, the above information is really a positive story. You have more people testing positive with really minimal symptoms. This means that the fatality rate is less than commonly reported.
Thus do we have first-hand confirmation of what we’ve suspected. So many of the new cases are among the young and so many of those infected have no symptoms or mild symptoms.
Previously we had less capacity to do testing and so many people with COVID-19 went undiagnosed. Now that we are doing more testing, more people who would have been undiagnosed are being diagnosed. Thus the upward trend in diagnosed cases. But the good news is that the deaths continue to decrease even as we find more previously undiagnosed cases.
This chart shows weekly death counts by age over the past few months. These decreases should be cause for cheer rather than cause for more lockdown.
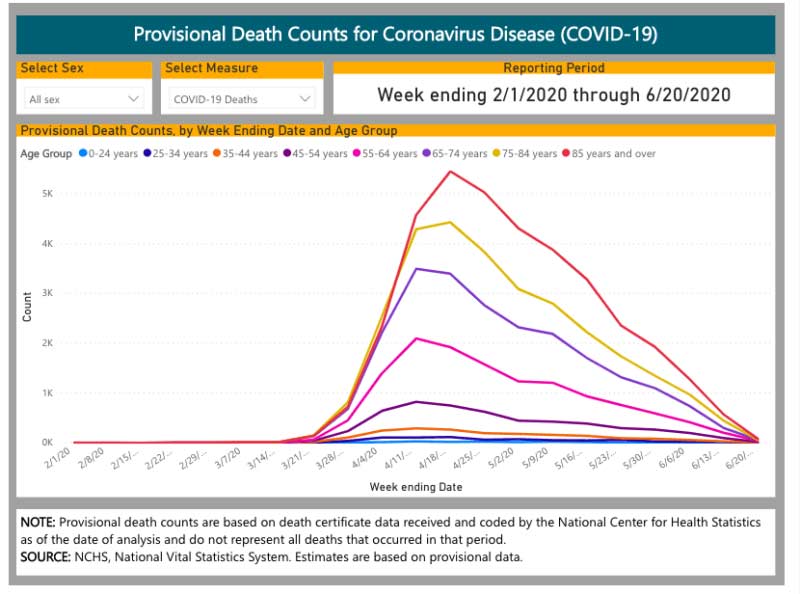
Source
It turns out that COVID-19 has a much lower fatality rate, especially among young people, when we include all of the previously undiagnosed cases.
The Centers for Disease Control Director Robert R. Redfield now estimates that about 20 million Americans have had and recovered from COVID-19. That means this deadly disease does not have a fatality rate of 6 percent but of 0.6 percent. And among young people the fatality rate is magnitudes lower than that.
The fact that increased testing means we are discovering more young and healthy people with COVID-19 should not be surprising or alarming in the slightest.
The hospitals are under financial pressure from having to mostly stop doing business for months, so they are classifying as many people as possible as a COVID case in order to gain the subsidy offered by the federal government. Overall, this is good news. Somehow, this is being spun as some kind of disaster that once again requires shutting down (though doing so will accomplish nothing).

Edward Peter Stringham is President of the American Institute for Economic Research, Davis Professor of Economic Organizations and Innovation at Trinity College, and Editor of the Journal of Private Enterprise. He is editor of two books and author of more than 70 journal articles, book chapters, and policy studies. His work has been discussed in 15 of the top 20 newspapers in the United States and on more than 100 broadcast stations including MTV. Stringham is a frequent guest on BBC World, Bloomberg Television, CNBC, and Fox. Rise Global ranks Stringham as one of the top 100 most influential economists in the world. He earned his B.A. from College of the Holy Cross in 1997, his Ph.D. from George Mason University in 2002. His book, Private Governance: Creating Order in Economic and Social Life, is published by Oxford University Press.
www.aier.org
|